In This Article
- Our Methodology
- Acknowledgments
- What is Neuropathy?
- How Common Is It to Treat Neuropathy with Medical Marijuana?
- How Effective is Medical Marijuana in Treating Neuropathy?
- What We Learned
- Medical Cannabis May Be as Effective as Opiates in Alleviating Pain for Some Neuropathy Patients
- Product Potency Matters More Than Dosage Size, Frequency, or Method of Consumption
- Studies Using Low Quality Cannabis Are Inherently Flawed
- Cannabis Has Fewer Negative Side Effects Than Other Neuropathy Treatments
- Underreporting of Neuropathy Has Far Reaching Consequences
Despite patients reporting that cannabis significantly reduces pain by over 30% for individuals with neuropathy, only ten states with medical cannabis programs explicitly list it as a qualifying condition. This information raises the question of whether or not patients are listing chronic pain as their condition or other related symptoms that states list as qualifying conditions. Another critical question this brings to light is how patient care may be affected due to the individualized nature of medical cannabis therapy for different conditions and symptoms. To better understand why patient outcomes and state policies are often in conflict and how this can limit patient access to safe and beneficial medicine, we surveyed 603 medical cannabis patients who were treating neuropathy as a primary or secondary condition.
Our Methodology
In our recent survey, the NuggMD team reached out to 603 patients to gather data on their use of cannabis as a treatment for neuropathic pain. Of these patients, 248 reported that they used cannabis as a primary treatment for neuropathic pain, while 355 said they used cannabis as a secondary treatment. It is important to note that participants were not offered incentives in exchange for participating in this survey.
The patients who participated in the study ranged from 18 to over 75 years old. Most patients who participated in the survey were between the ages of 45 and 64. In terms of gender identification, 292 of the patients identified as female, and 304 identified as male. There were also three patients who identified as non-binary and four who chose not to disclose their gender.
It's important to note that our survey does not provide causal evidence of cannabis being effective in the treatment of neuropathic pain. However, this survey does add to the large body of evidence that supports other studies and anecdotal reports on cannabis as a treatment for neuropathic pain. Our survey results suggest a great need for further research to be focused explicitly on neuropathic pain and its potential treatment with cannabis.
Acknowledgments
| Alexandra Arnett Report Author, Researcher & Writer at NuggMD University of Maryland School of Pharmacy, Master of Science in Medical Cannabis Science and Therapeutics Tyler Elson Report Analyst & Editor, Content Marketing Manager at NuggMD Deb Tharp Report Analyst & Fact Checker, Lead Legal Researcher at NuggMD | Dr. Brian Kessler Report Medical Review, Medical Provider and Medical Reviewer at NuggMD Pain Management & Sports Medicine St. George’s University School of Medicine, New York Medical College, Lincoln Hospital Medical Center, Residence in General Surgery Medical License in NY and CA Member of the American Medical Association (AMA) |
What is Neuropathy?
Neuropathy is a group of conditions that involve damage to the nervous system. There are over 100 types of neuropathy, and the symptoms vary depending on the damaged nerve type and whether it is motor, sensory, or autonomic. Neuropathic pain is a chronic pain condition for many individuals and can be caused by a variety of factors, including but not limited to:
- Diabetes
- Autoimmune disorders
- Vitamin deficiencies
- Alcoholism
- Medications
- Cancer treatments
- Viral infections
- Genetic disorders
- Injury
- Aging
People with neuropathy may experience one or more of the following symptoms, depending on the type of nerve damage they have:
- Numbness
- Burning, stabbing, freezing, or tingling pain
- Muscle weakness, especially in legs, feet, arms, or hands
- Unusual or increased sensation or extreme sensitivity to touch
- A feeling that you’re wearing socks or gloves when you’re not
- Difficulty walking, running, or controlling arm movements
- Trouble with balance and coordination
- Difficulty holding things
- Foot dragging, also called foot drop
- Unusually high arches
- Curled toes (hammer toes)
How Common Is It to Treat Neuropathy with Medical Marijuana?

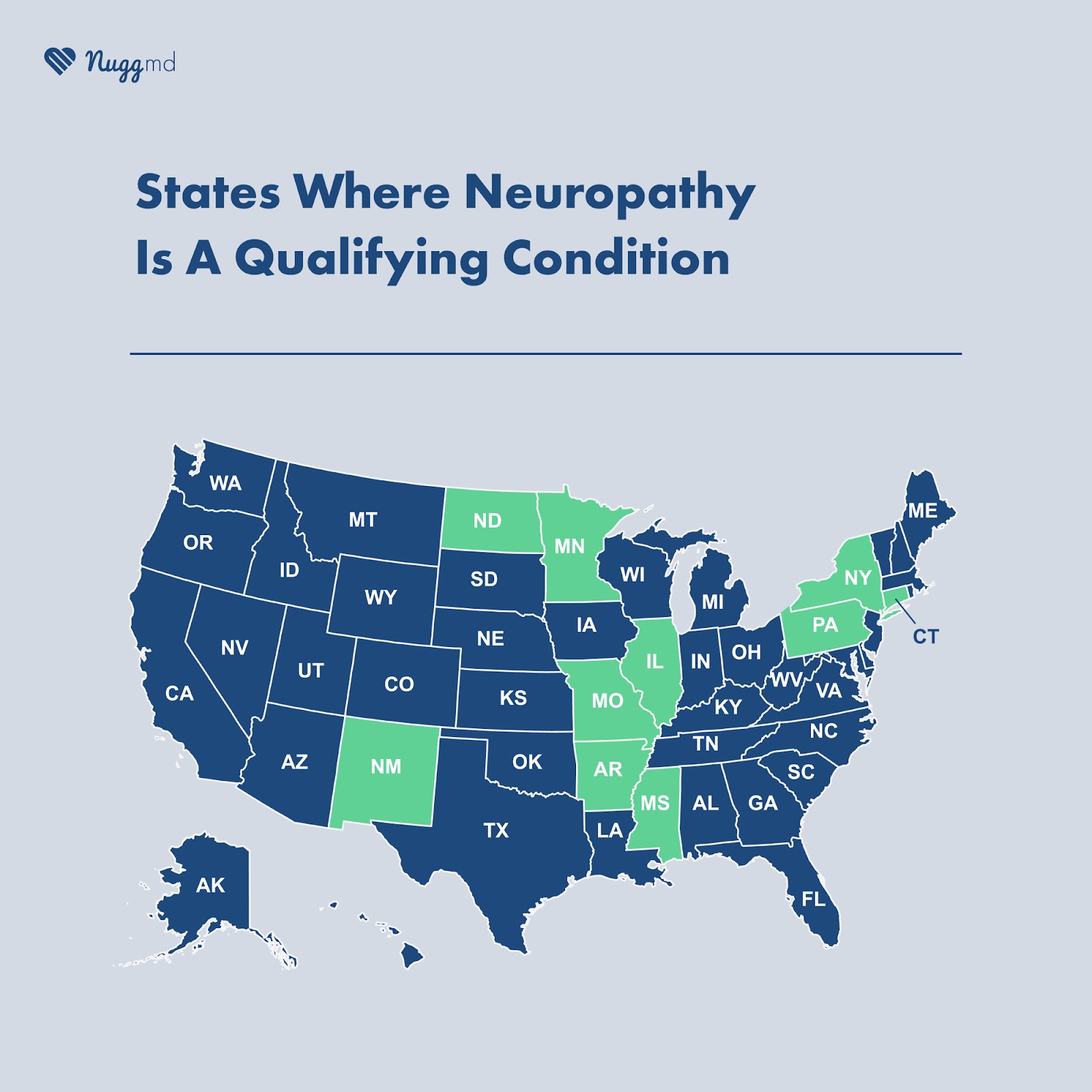
Over 20 million individuals in the United States are suffering from some form of peripheral neuropathy, according to the National Institute of Neurological Disorders and Stroke; however, out of 38 states with medical cannabis programs, only ten explicitly list neuropathy as a qualifying condition. Although pain is one of the most common symptoms of neuropathy, according to our 2022 Cannabis Conditions Report, merely 1.91% of patients report using cannabis to treat neuropathy.
In our survey, 520 of 603 respondents (86.2%) reported pain levels of over 6 (on a 10-point scale) before using medical cannabis. Many patients seek cannabis for chronic pain resulting from neuropathy, as pain is the most common and debilitating symptom. Because patients are often forced to choose chronic pain or another symptom as their qualifying condition to obtain a medical cannabis card instead of neuropathy, this skews the data resulting in an unclear picture of how many medical cannabis patients are using it for neuropathy. However, based on national figures, we can give general estimates.
In the United States, neuropathy is estimated to affect more than 20 million people, while chronic pain affects 50.2 million adults. In states with medical cannabis laws, chronic pain is the qualifying condition most commonly reported among medical cannabis patients. According to data from NORML, they estimate that over 65% of medical cannabis patients used chronic pain as a qualifying condition to enroll in their state’s medical cannabis program. In addition, our 2022 Conditions Report found that 26.3% of patients use cannabis for chronic pain.
Based on this data, if we were to estimate that medical cannabis patients are diagnosed with neuropathy or chronic pain at rates comparable with the national estimates, we could make an educated guess that the number of medical cannabis patients who are seeking to use cannabis for treating neuropathy are significantly higher than the 1.91% reported in our survey. The data in our 2022 Conditions Report shows that within the United States, neuropathy is roughly 40% less common in the United States than chronic pain. This data suggests that approximately 10.5% of patients seeking a medical cannabis card do so to alleviate neuropathy or symptoms related to the condition, like chronic pain.
How Effective is Medical Marijuana in Treating Neuropathy?

In our survey of 603 individuals who use cannabis for medical purposes, 248 participants reported that neuropathy was the primary condition they were treating with cannabis. An additional 355 respondents listed neuropathy as a secondary condition for which they were using cannabis, which may be because neuropathy was not a qualifying condition in their state. They may instead have obtained a medical card for a symptom such as chronic pain. The ages of the respondents ranged from 18 to over 75, with the majority falling between the ages of 45 and 64. Our survey found that 50.4% of participants identified as male and 48.4% as female.
Pro-inflammatory agents, such as cytokines and histamines, have been shown to produce pain. Current research has demonstrated that cannabinoid receptor agonists, such as THC, have the ability to block pain and reduce neuro-inflammation. Additionally, research has also indicated that pain can be reduced by increasing the body’s natural endocannabinoid levels. Increasing the body’s natural endocannabinoid levels can be done, for example, by using CBD to boost anandamide levels. Both THC and CBD seem to be able to reduce neuropathic pain, but CBD may produce fewer unwanted side effects. Overall, the potential benefits of cannabinoid receptor agonists like THC and natural endocannabinoid boosters like CBD for pain management are meaningful and warrant continued research.
What We Learned

Medical Cannabis May Be as Effective as Opiates in Alleviating Pain for Some Neuropathy Patients
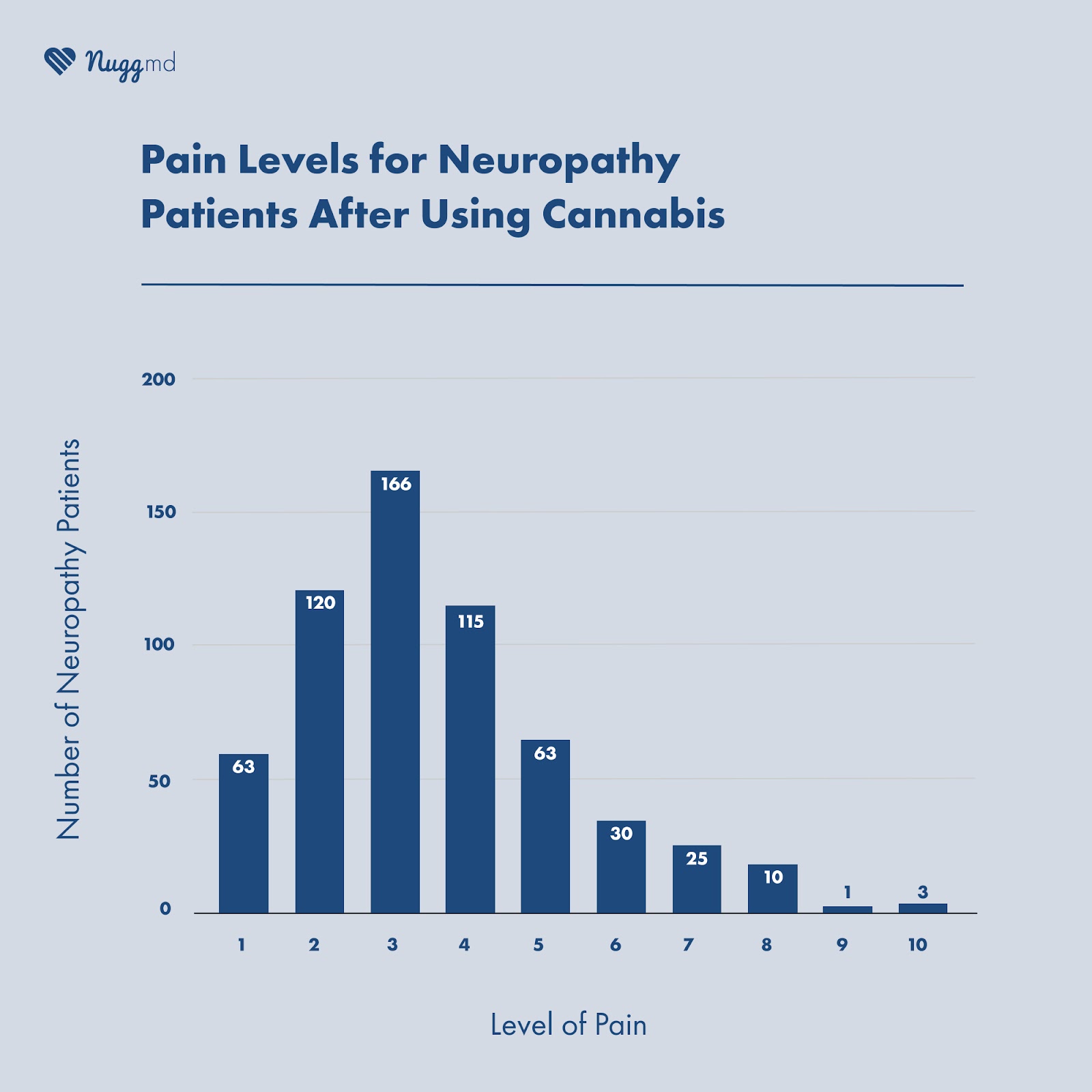
A total of 596 participants provided their levels of pain relief before and after using cannabis. Based on a 10-point scale, the average pain level before cannabis use was 7.64, while the average pain level after cannabis use was 3.44. This data demonstrates an average pain relief level of 4.2 out of 10 for participants.
Out of 596 participants who reported their pain levels before and after using cannabis, 520 participants described having a pain level of six or higher on a 10-point scale before using cannabis.
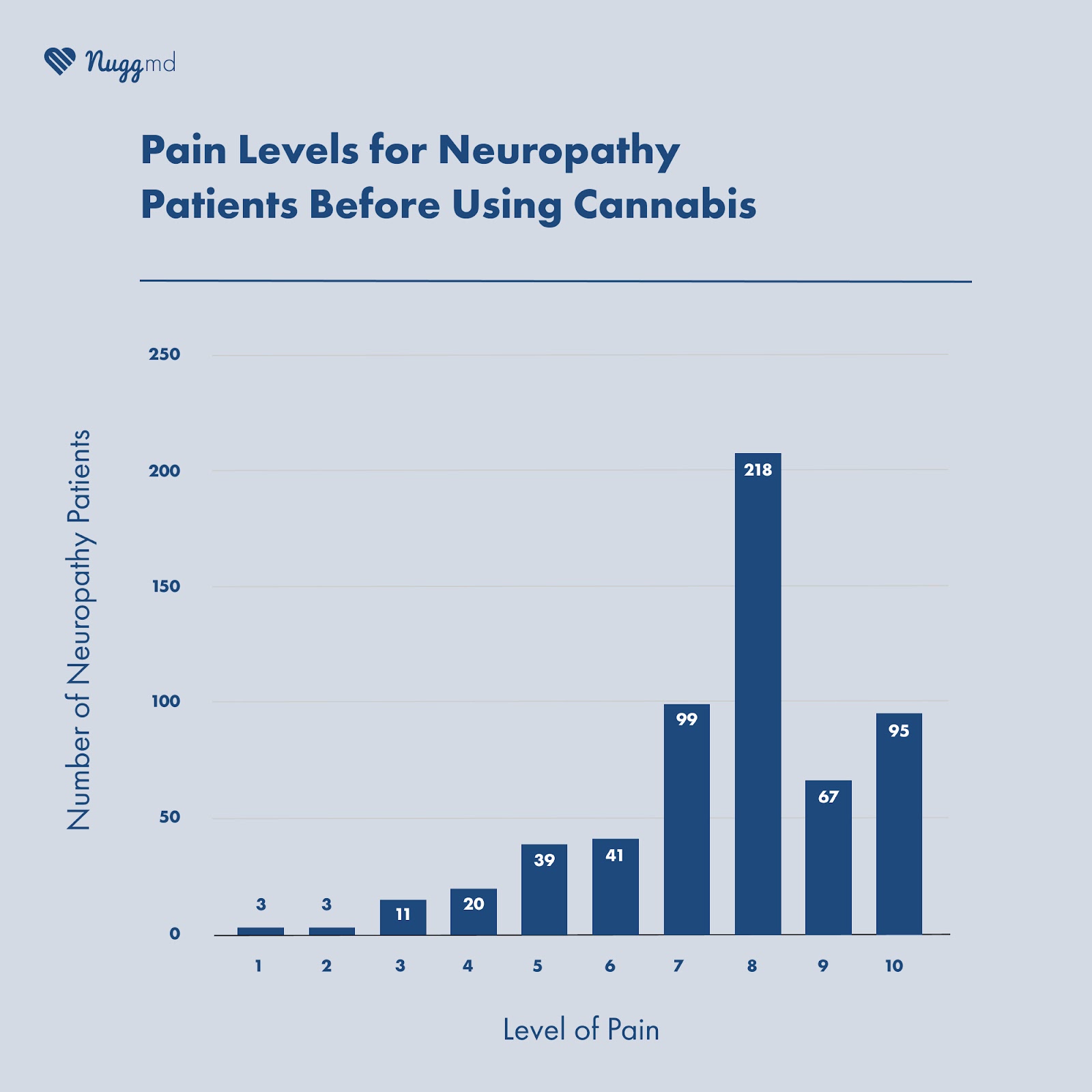
And of the 520 patients who started with pain levels of six or higher before using cannabis, 269 reported pain levels of three or below after using cannabis. In comparison, 69 patients remained at a six or higher after cannabis use, 8 said they had no relief from cannabis, and 7 reported having increased pain levels.
In our study, we found a 4.2 point average reduction in pain when individuals used cannabis. This number is similar to the pain reduction that is experienced by individuals who use opiates. A 2017 randomized clinical trial of 411 patients from an emergency department with acute pain in extremities rated their pain an 8.7 on an 11-point scale. Patients received a single dose of either opioid or nonopioid pain medication and reported their pain scores after. On average, pain decreased by the following;
- 4.3 with ibuprofen and acetaminophen
- 4.4 with oxycodone and acetaminophen
- 3.5 with hydrocodone and acetaminophen
- 3.9 with codeine and acetaminophen
These results suggest that opiates were not significantly more effective than using a combination of ibuprofen and acetaminophen to relieve pain.
While our report's findings demonstrate that the use of cannabis at the right potency and dosage shows promise toward treating chronic pain conditions such as neuropathy, more research is needed to determine safety and efficacy. Individuals seeking to use cannabis for chronic pain or neuropathy should seek the advice of a reputable cannabis doctor or nurse before making any changes to their current treatment regimen.
Product Potency Matters More Than Dosage Size, Frequency, or Method of Consumption
According to our survey, there was no correlation between the method of consumption and the levels of pain relief that individuals were experiencing. Out of 603 total respondents, 155 stated that they use the doctor-recommended form of consumption. However, 446 respondents noted that they use the method of ingestion they prefer instead of the doctor-recommended form. The following is a breakdown of how these 446 individuals consumed their medical cannabis;
- 137 inhaled only
- 101 inhaled, used edibles and topicals
- 88 used edibles only.
- 22 used topicals and inhaled.
- 18 used edibles and topicals.
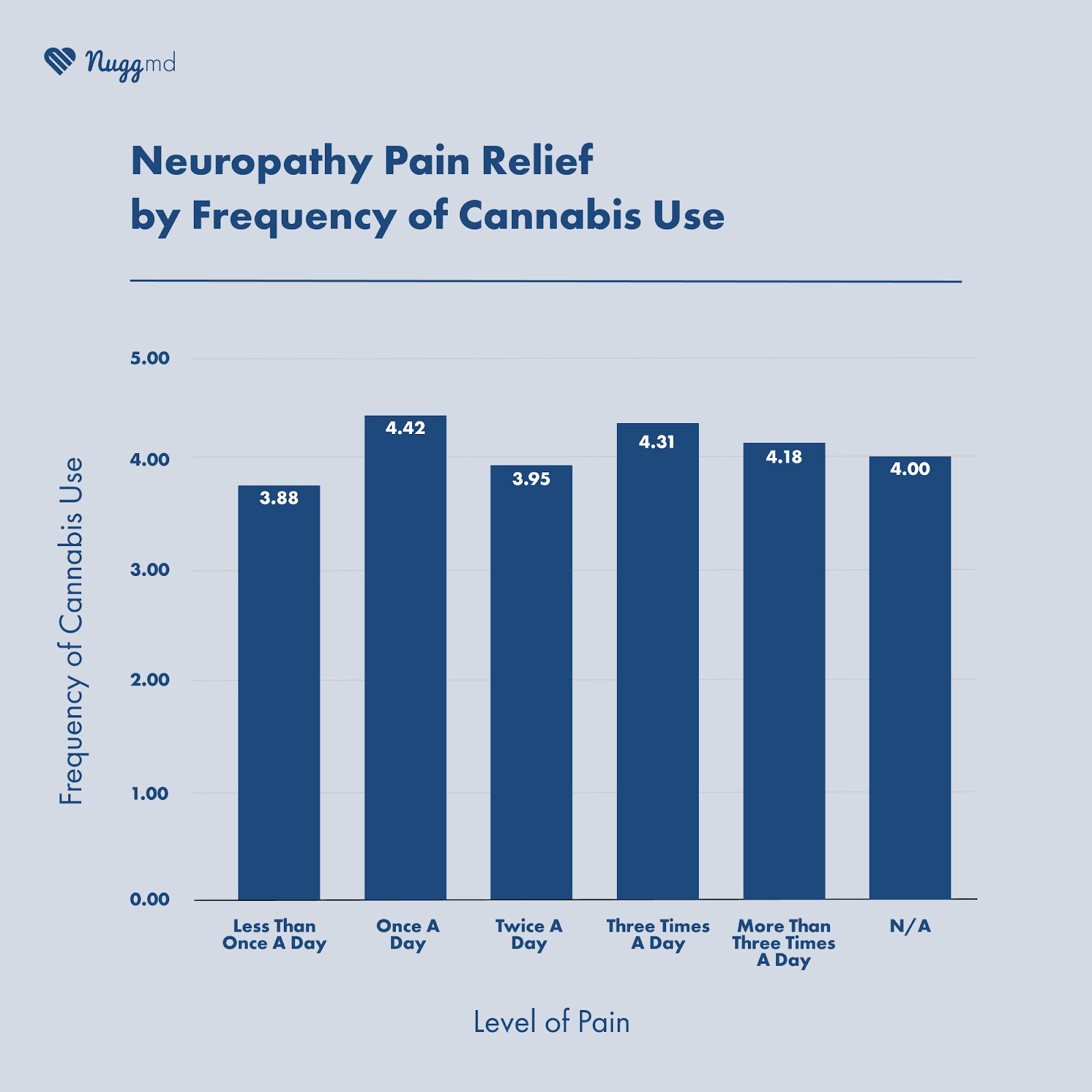
In addition, our survey found that increasing the dosage of cannabinoids did not necessarily lead to more effective relief. In fact, 64.3% of participants reported that the recommended dosage was enough to alleviate their symptoms. However, 18.2% of participants disagreed with this recommendation. Similarly, most respondents (65.7%) reported not exceeding the prescribed amount, while only 20.1% admitted to using more. Additionally, we found no significant correlation between the number of cannabis sessions per day and the level of pain relief experienced by participants.
It is worth noting that the majority of patients who reported using inhaled cannabis products consumed products with a THC concentration that exceeded 20%. Our survey found that a small percentage, 11.1% of participants, used inhalable cannabis products with less than 20% potency, and only 3.9% of participants did not use inhalable cannabis products.
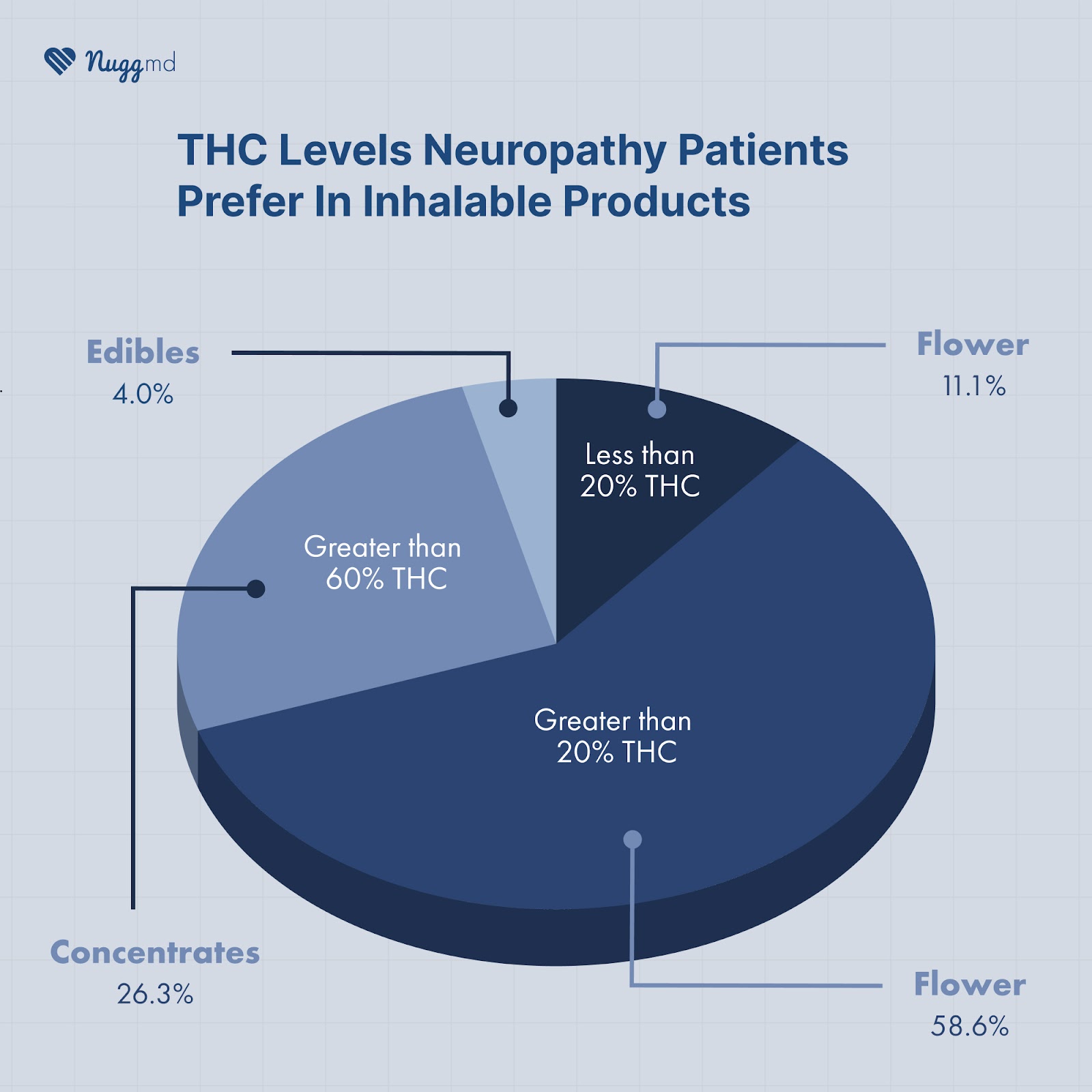
Although our survey found that cannabis provided relief for many individuals, the method of consumption and frequency of use varied considerably among the participants. According to our survey, the most constant variable was the use of high-potency cannabis with a THC content of 20% or more. This finding is important to note because much of the research on the efficacy of cannabis for pain typically involves cannabis products with a potency below 20% THC. These research studies often result in claims that THC is ineffective for pain relief.
Studies Using Low Quality Cannabis Are Inherently Flawed
Our survey results demonstrated that individuals using high-THC cannabis found more significant pain relief for their neuropathy. However, much of the research on cannabis as a treatment for neuropathy uses low-quality cannabis with low THC levels, focus on CBD, or uses isolated compounds and not full-spectrum products. These products often used in research are not representative of what medical cannabis patients are obtaining on the recreational and medical markets.
An analysis of the below articles indicates the importance of using quality cannabis when examining the effects of cannabinoids on pain. While none of the studies stated the cannabinoid levels of the cannabis used, it was primarily provided by the National Institute on Drug Abuse Drug Supply Program; however, one study did obtain cannabis from the National Cancer Institute. Because government-grown cannabis is typically low-quality and low in THC compared to what the recreational and medical cannabis markets have, the lack of pain relief these researchers observed may be due to the low quality and low THC differences. Our analysis also included a study from 1974 to demonstrate the difference in cannabinoid levels of older cannabis compared to modern cannabis.
Several studies have been conducted over the last several decades to evaluate the efficacy and safety of cannabinoid-based medicine for pain treatment. In 2007, Wallace et al. conducted a study and found that smoked cannabis showed no significant reduction in capsaicin-induced pain and hyperalgesia in healthy participants. Similarly, another study conducted by Wallace et al. (2015), consisting of thirty participants, found that when compared to a placebo, cannabis did not reduce pain in patients with diabetic neuropathy. Another early study from 2007 by Abrams et al. which included individuals who had HIV-associated sensory neuropathy, demonstrated that cannabis did not significantly reduce pain compared to a placebo. Wisley et al. conducted a study in 2008 that compared “cannabis cigarettes” to a placebo, and their research found that there was no significant reduction in neuropathic pain in patients. In 2011, Abrams et al. conducted another study and found that compared to a placebo, inhaled cannabis did not result in substantial reductions in pain for chronic pain patients.
In 2010, Markman et al. conducted a study using cannabis obtained from the National Cancer Institute. The team examined an oral mucosal cannabinoid extract for treating chemotherapy-induced neuropathic pain. The researchers found no significant reduction when using the cannabinoid extract compared to a placebo. The oldest study we looked at by DuPont and Jaffe was from 1974, which indicates that the cannabis used in the study was of very low quality and likely very little THC. The researchers found that smoked cannabis, when compared to a placebo, had no significant effect on the pain levels of cancer patients in the hospital.
More recent studies on cannabis and pain have participants using higher-quality, high-THC cannabis due to the large availability of recreational and medical cannabis products on the present market. In addition, more studies are using cannabinoid isolates in high doses and examining the effects of different cannabinoid ratios on pain, including the use of full-spectrum cannabis products. These factors are important to recognize as we continue to research cannabis for the treatment of neuropathy.
Cannabis Has Fewer Negative Side Effects Than Other Neuropathy Treatments
Based on previous research findings, cannabis provided similar levels of pain relief when compared to placebo or alternative treatments. Out of the 603 individuals who participated in the survey, only a small number of them, 18, reported adverse side effects from cannabis. Adverse side effects of cannabis can include:
- Anxiety
- Dry mouth
- Dizziness
- Increased appetite
- Increased heart rate
- Paranoia
In our survey, we also asked respondents about other prescription medication treatments they had used for pain relief before turning to cannabis. Out of the respondents, 321 reported having tried opiates or tramadol. Additionally, 252 patients reported having stopped these other treatments due to adverse side effects. Side effects of prescription medication like opiates and tramadol include:
- Constipation
- Drowsiness
- Hallucination
- Nausea
- Respiratory Depression
- Sedation
- Vomiting
Besides the above-mentioned adverse side effects of opiates and tramadol, it is crucial to note that both drugs can cause death if taken in excessive doses. In contrast, cannabis alone has almost no risk of death and overall has significantly fewer adverse side effects. This fact is highlighted by the data we collected, that 41.7% of survey participants reported experiencing an enhanced quality of life after stopping the use of opiates or tramadol and switching to cannabis.
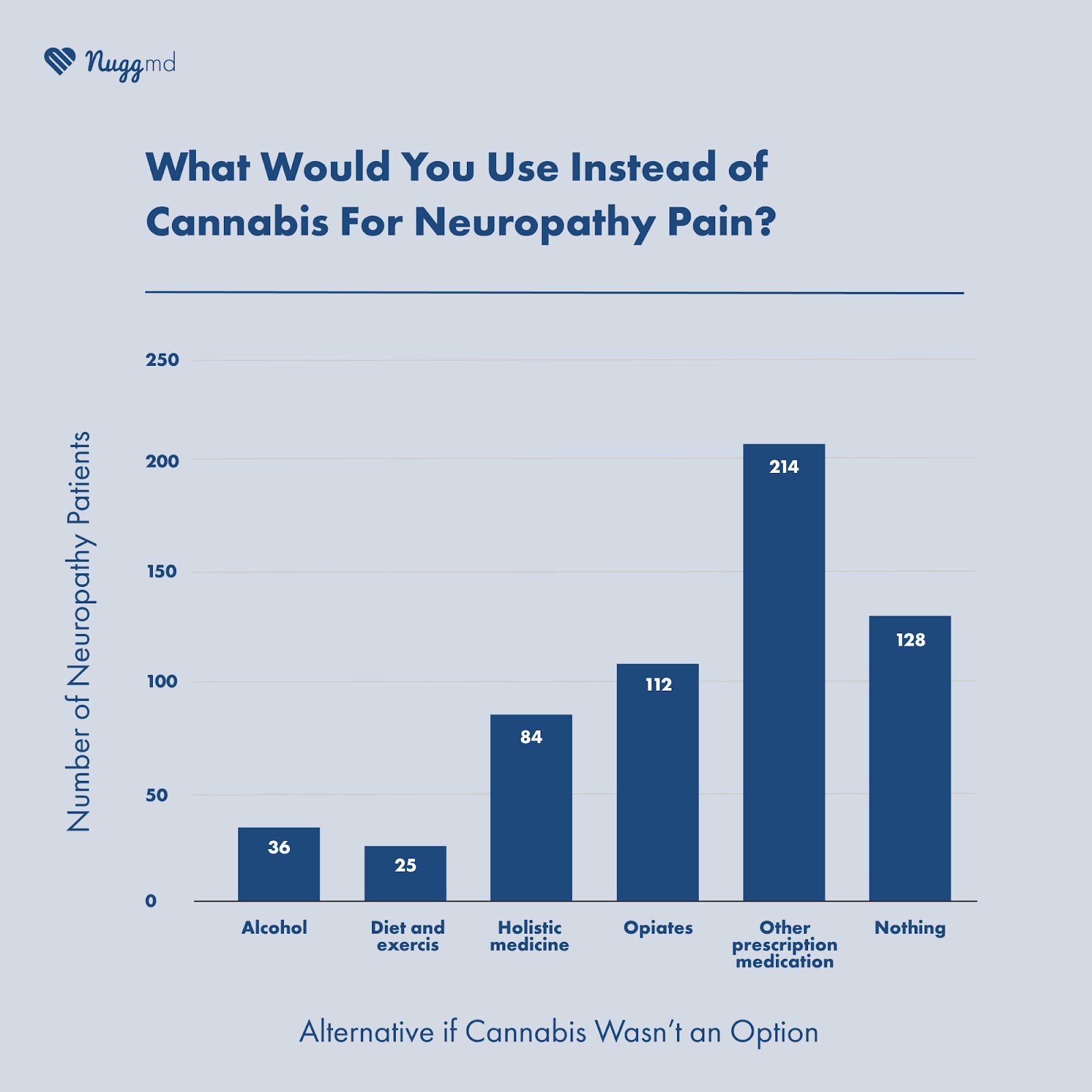
In our survey, we asked patients what they would do if they could no longer access cannabis and 60% of individuals responded that they would turn to opiates, alcohol, or other prescription medications. Compared to cannabis, these alternatives cause adverse effects such as dependence or, in some cases, death.
Of the 603 survey respondents, 113 stated they would choose prescription opiates, 214 said they would use other prescription medication, and 36 stated they would use alcohol as an alternative to cannabis if they did not have access, even though alcohol is known to cause neuropathy in some users. Furthermore, 128 individuals said they would not replace cannabis with any alternative medication or drug if they could no longer access their medicine. This data indicates that 21.2% of neuropathy patients would rather tolerate the symptoms of their condition than deal with the side effects and potential dependency that can come with alternative treatment methods such as opiates.
“Neuropathy is a chronic condition needing long-term treatment,” says Dr. Brian Kessler, NuggMD’s Chief Medical Officer. “I hear from many patients who are worried about the risk of severe side effects and dependence when using opioids and drugs like gabapentin over extended periods of time. For many patients, medical marijuana offers a safer alternative that improves their quality of life.”
Underreporting of Neuropathy Has Far Reaching Consequences
All but one state with medical cannabis programs mentions pain explicitly as a qualifying condition for a medical cannabis recommendation. This means that, between severe and chronic pain and muscle spasms, many individuals with neuropathy are eligible to obtain medical cannabis in states with medical cannabis programs. Interestingly, there are only ten states that list neuropathy specifically as a qualifying condition for medical cannabis.
The national prevalence of neuropathy in adults is nearly 17% of the United States population, but only 1.91% of patients report that neuropathy is why they choose to use medical cannabis. Based on our survey, 21.2% of individuals would decide not to replace cannabis with another treatment if they did not have access to medical cannabis. This data suggests that states who do not explicitly list neuropathy as a qualifying condition for medical cannabis could be limiting access for up to 1 in 5 neuropathy patients who believe they are unable to obtain a recommendation due to their condition not being listed.
In addition, the data collected on medical cannabis patients from states that do not explicitly list neuropathy as a qualifying condition could skew research on medical cannabis and neuropathy. By forcing individuals to choose chronic pain as their qualifying condition, which is just a symptom, instead of neuropathy, the actual condition, we limit the funding and effort put toward researching the subject. Research on chronic pain and cannabis is prevalent, and while many of these studies include patients with neuropathy, very little research exists to look at patients with pain explicitly due to neuropathy.
Furthermore, the lack of research using products that resemble what is on the medical and recreational markets, such as products with an array of cannabinoid and terpene ratios, high-THC products, and the variety of consumption methods, leaves us in the dark about the true efficacy of using medical cannabis to treat neuropathy. Since the effects of medical cannabis can vary greatly from patient to patient, this lack of research is detrimental to patient outcomes.
Research that has used cannabis products that are on par in quality with recreational and medical cannabis products on the market, whether it be high THC or high CBD, suggests that medical cannabis is effective in treating neuropathic pain. Our survey found that neuropathy patients had more than a 30% reduction in pain when using cannabis. We find that the lack of inclusion of neuropathy in cannabis research is inconsistent with our available data.
The information in this article and any included images or charts are for educational purposes only. This information is neither a substitute for, nor does it replace, professional legal advice or medical advice, diagnosis, or treatment. If you have any concerns or questions about laws, regulations, or your health, you should always consult with an attorney, physician or other licensed professional.